Our Hyperacusis and Misophonia Program
We provide a unique, individualised program to assist you in achieving increased tolerance to everyday sound, with Philippa James utilising established experience and research in hyperacusis and misophonia therapy. Our program is part of a holistic multidisciplinary team, working with uniquely skilled and experienced physiotherapists, psychologists, a hypnotherapist and pain physicians.
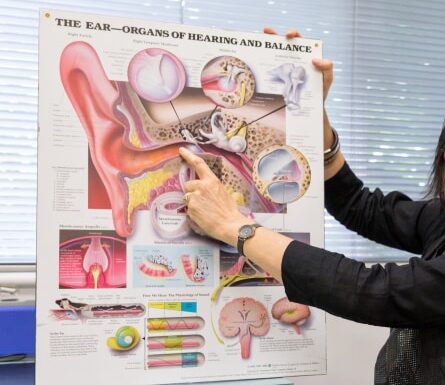
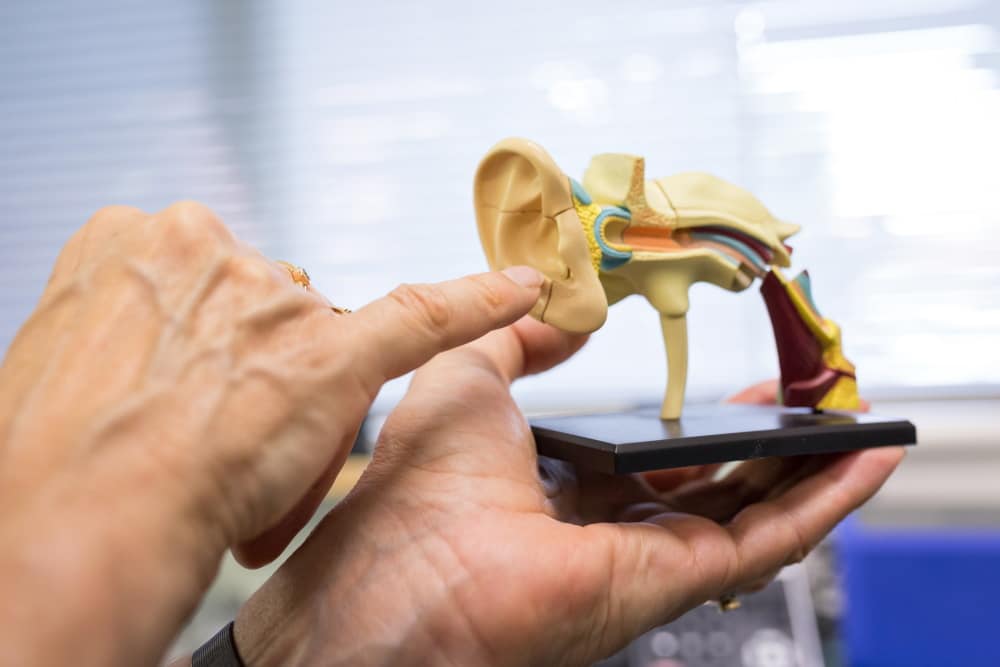
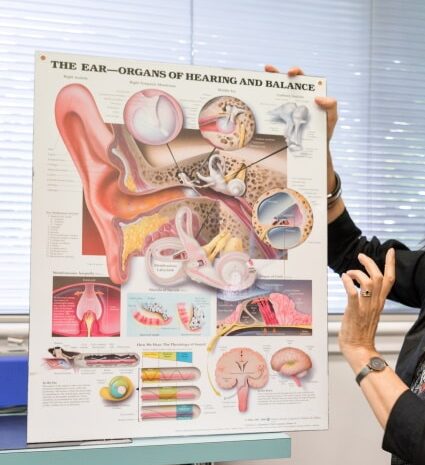
A detailed description of the peripheral (the outer, middle and inner ear) and central (the brain) auditory pathway is essential to understand how hyperacusis and/or misophonia develops.
Our Program involves:
- an evaluation of your hyperacusis and/or misophonia and its impact on you.
- providing a detailed understanding about the development of your hyperacusis and/or misophonia.
- a personalised explanation of the peripheral and central auditory system, including the neurophysiological basis of hyperacusis/misophonia and TTS (if symptoms are present).
- a hyperacusis/misophonia therapy program.
It has been our experience that once patients understand how the brain processes sound and understand in depth how their hyperacusis/misophonia developed, they have a possible pathway for reversal utilising the concepts of brain plasticity. This understanding provides reassurance, relief and insight, and is often helpful at relieving the suffering, distress, anxiety and bewilderment that tends to accompany both hyperacusis and misophonia, as well as the guilt, shame and anger that often accompanies misophonia.